Understanding how bacterial hideouts form and flourish is crucial for anyone serious about gum disease prevention. For health-conscious individuals exploring cutting-edge oral care solutions, the science behind periodontal pocket formation reveals why conventional brushing and flossing often fall short, and why advanced therapeutic approaches are revolutionising oral healthcare.
Your mouth harbours a hidden battlefield where microscopic invaders establish fortified colonies in the deepest recesses of your gums. These bacterial sanctuaries, known as periodontal pockets, represent one of the most sophisticated survival strategies in the microbial world. Unlike the visible plaque on tooth surfaces, these subgingival environments create perfect conditions for pathogenic bacteria to thrive, protected from traditional cleaning methods and your body’s natural defences.
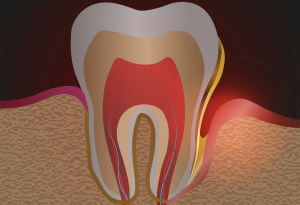
What are periodontal pockets and how do they form?
In healthy mouths, your gums form a protective seal around each tooth, creating a shallow groove called the gingival sulcus. This natural space typically measures between 1 and 3 millimetres deep, serving as the frontier between your oral environment and the deeper tissues that support your teeth.
The transformation from healthy sulcus to pathological pocket begins with bacterial accumulation. When plaque bacteria establish themselves along the gumline, they release toxins and inflammatory mediators that trigger your immune system’s response. However, this defensive reaction inadvertently creates the very environment these bacteria exploit.
As inflammation progresses, the gum tissue begins to separate from the tooth surface, creating deeper spaces. Bacterial toxins break down the connective tissue fibres that normally anchor your gums to your teeth, whilst inflammatory enzymes destroy the supporting bone structure. This process creates pockets deeper than 4 millimetres, with severe cases reaching depths of 7 millimetres or more.
The irony of periodontal disease lies in how our body’s attempt to fight infection actually creates the perfect environment for bacteria to establish permanent colonies.
How bacterial biofilms colonize subgingival environments
The microbiology of subgingival colonisation represents a masterclass in bacterial adaptation. Unlike the aerobic bacteria that dominate tooth surfaces, periodontal pockets become increasingly anaerobic as they deepen, creating distinct ecological niches.
Biofilm formation begins with early colonisers like Streptococcus species, which create the foundation for more complex bacterial communities. These initial settlers produce a protective matrix of proteins and polysaccharides, essentially building a microscopic city with sophisticated infrastructure.
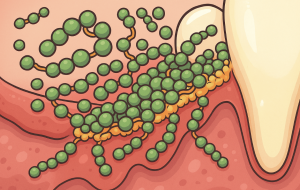
As the biofilm matures, bacterial succession occurs in predictable patterns. Gram-positive species give way to gram-negative anaerobes, including notorious pathogens like Porphyromonas gingivalis and Tannerella forsythia. These late colonisers possess sophisticated virulence factors, allowing them to evade immune responses and actively destroy host tissues.
The subgingival environment provides everything these bacteria need to thrive: protection from oxygen, a steady supply of nutrients from gingival fluid, and minimal mechanical disruption. The biofilm structure creates gradients of oxygen and pH, allowing different bacterial species to occupy their preferred microenvironments within the same pocket.
Why traditional cleaning methods fail in deep pockets
Even the most diligent oral hygiene routine faces significant limitations when confronting established periodontal pockets. Research indicates that even the best toothbrushes remove only 65% of plaque, leaving substantial bacterial populations intact, particularly in deeper spaces where bristles cannot reach.
The biofilm resistance mechanisms present perhaps the greatest challenge. The protective matrix surrounding bacterial colonies acts like armour, reducing the penetration of antimicrobial agents by up to 1000-fold compared to planktonic bacteria. This means that mouthwashes and other topical treatments often fail to achieve therapeutic concentrations where they’re needed most.
Physical accessibility represents another fundamental barrier. Periodontal pockets create tortuous pathways that prevent effective mechanical cleaning. The anatomy of these spaces, combined with inflammation and bleeding, makes it virtually impossible for conventional tools to reach the deepest bacterial colonies.
The anaerobic environment within pockets also protects bacteria from oxygen-based antimicrobial mechanisms. Many traditional oral care products rely on oxidative stress to eliminate bacteria, but these mechanisms become ineffective in the oxygen-depleted depths of periodontal pockets.
Advanced therapeutic approaches for pocket decontamination
Photodynamic therapy represents a paradigm shift in treating these bacterial sanctuaries. This approach uses light-sensitive compounds that selectively bind to bacterial cells and biofilms. When activated by specific wavelengths of light, these photosensitisers generate reactive oxygen species that can penetrate biofilm matrices and eliminate bacteria with remarkable precision.
The science behind light-activated therapies addresses many limitations of conventional treatments. Unlike broad-spectrum antimicrobials that disrupt beneficial oral flora, photodynamic therapy can be precisely targeted to pathogenic species whilst preserving the healthy microbiome balance essential for oral health.
Modern dual-light systems combine different wavelengths to achieve multiple therapeutic goals simultaneously. Blue light around 405 nanometres provides direct antibacterial effects, whilst near-infrared wavelengths support tissue healing and reduce inflammation. This approach not only eliminates bacterial colonies but also promotes the restoration of healthy periodontal architecture.
The effectiveness of these advanced approaches lies in their ability to overcome biofilm protection mechanisms. Light penetrates the bacterial matrix more effectively than chemical agents, whilst the localised generation of reactive species ensures high concentrations precisely where they’re needed. This targeted approach represents a significant advancement in gum disease prevention and treatment.
For individuals exploring the bad breath paradox or seeking to understand why persistent bad breath occurs, addressing these hidden bacterial sanctuaries often provides the root-cause solution that conventional approaches miss.
Understanding periodontal pocket formation and the sophisticated bacterial communities they harbour illuminates why traditional oral care often falls short. As we continue to unravel the complex relationships between oral and systemic health, targeted therapeutic approaches offer new hope for preventing and treating these hidden bacterial sanctuaries that threaten both oral and overall wellbeing.

